Integrating Nutraceuticals into Allergy Management for Children: A Guide for Healthcare Professionals
Posted on February 7, 2024 • 7 minutes • 1390 words
Table of contents
Allergy-related conditions are highly prevalent, encompassing a range of disorders such as allergic rhinitis (AR) — the most frequently observed IgE -mediated condition, along with allergic asthma, food allergies, drug allergies, and reactions to insect stings. These conditions can trigger a broad array of symptoms, from minor itching to severe, potentially fatal, anaphylactic reactions . At the core of allergic diseases is a type 2 inflammatory response , marked by an eosinophilic infiltration in the nasal mucosa. The persistence of this type of immune reaction is linked to a specific, yet reversible, malfunction in T regulatory cells. Initially, this phenomenon was thought to be explained by the hygiene hypothesis , but recent insights have led to its reevaluation and the proposal of the microbiota hypothesis. Essentially, imbalances in the gut and respiratory microbiota can influence the development of a child’s immune system, promoting a type 2 immune orientation. Interestingly, this type 2 immune response begins even before birth, as a mechanism by the mother to prevent rejection of the fetus, leading to an initial type 2 bias in the newborn that must be corrected as the immune system matures toward a more balanced type 1 immunity .
| Type 2 allergy mechanism |
|---|
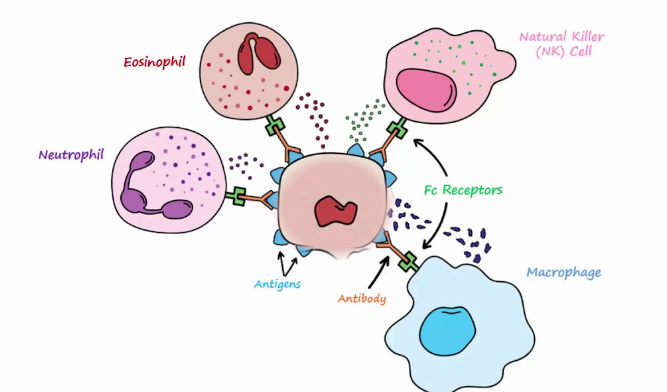 |
In individuals with allergies, there’s an increase in T helper 2 lymphocytes that leads to the production of type 2 cytokines , including interleukin four (IL-4), IL-5, and IL-13. These cytokines play a dual role: they not only cause an isotypic shift towards IgE production but also drive eosinophilic inflammation. Consequently, exposure to the specific allergen triggers allergic inflammation in these individuals. This type of inflammation will continue as long as the individual is exposed to the allergen that causes their reaction.
| Eosinophile |
|---|
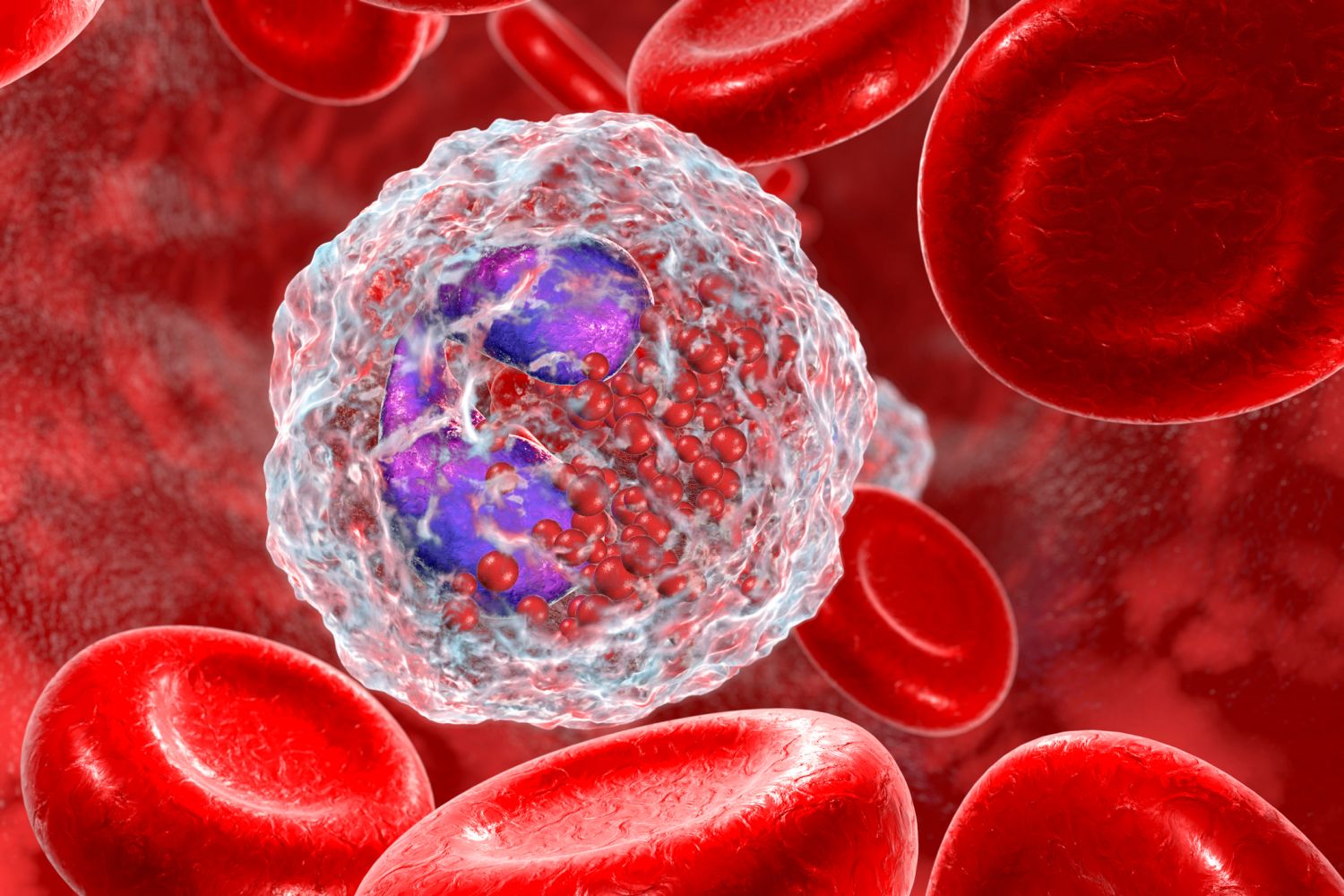 |
The significance of these inflammatory processes lies in their role in causing and maintaining allergic symptoms. For instance, the common symptoms of allergic rhinitis are nasal itching, sneezing, runny nose, and nasal blockage. In the case of asthma, symptoms include wheezing, shortness of breath, coughing, and a feeling of tightness in the chest. Meanwhile, food allergies, as well as reactions to venom and medications, can manifest in a variety of ways, further highlighting the complexity and variability of allergic responses.
Symptoms of allergies often appear immediately following exposure to an allergen, in what is referred to as the early phase. This immediate response is primarily due to the release of mediators like histamine . Following this initial phase, type 2 inflammation sets in, leading to a variety of other symptoms that are typical of allergic conditions. These include nasal and bronchial blockage, diminished sense of smell, hives, and general bodily discomfort.
| Allergy |
|---|
 |
Additionally, some individuals with allergies may experience a mild fever, indicative of a systemic inflammatory response. This is why allergic rhinitis was historically termed “hay fever.” Beyond the direct symptoms, allergic disorders have a significant negative impact on the quality of life for those affected. Consequently, allergies pose a considerable challenge not only to the individual sufferers and their families but also to society at large due to the broad range of effects and the potential for severe reactions.
Moreover, it’s common for individuals with allergies to have comorbid conditions, which can include other forms of allergic reactions such as conjunctivitis, rhinitis, asthma, food allergies, and drug allergies, as well as a higher susceptibility to infections. This complexity often necessitates a comprehensive approach to management and treatment to address both the allergies themselves and any associated conditions.
| Asthma: inflamed vs normal bronchial tube |
|---|
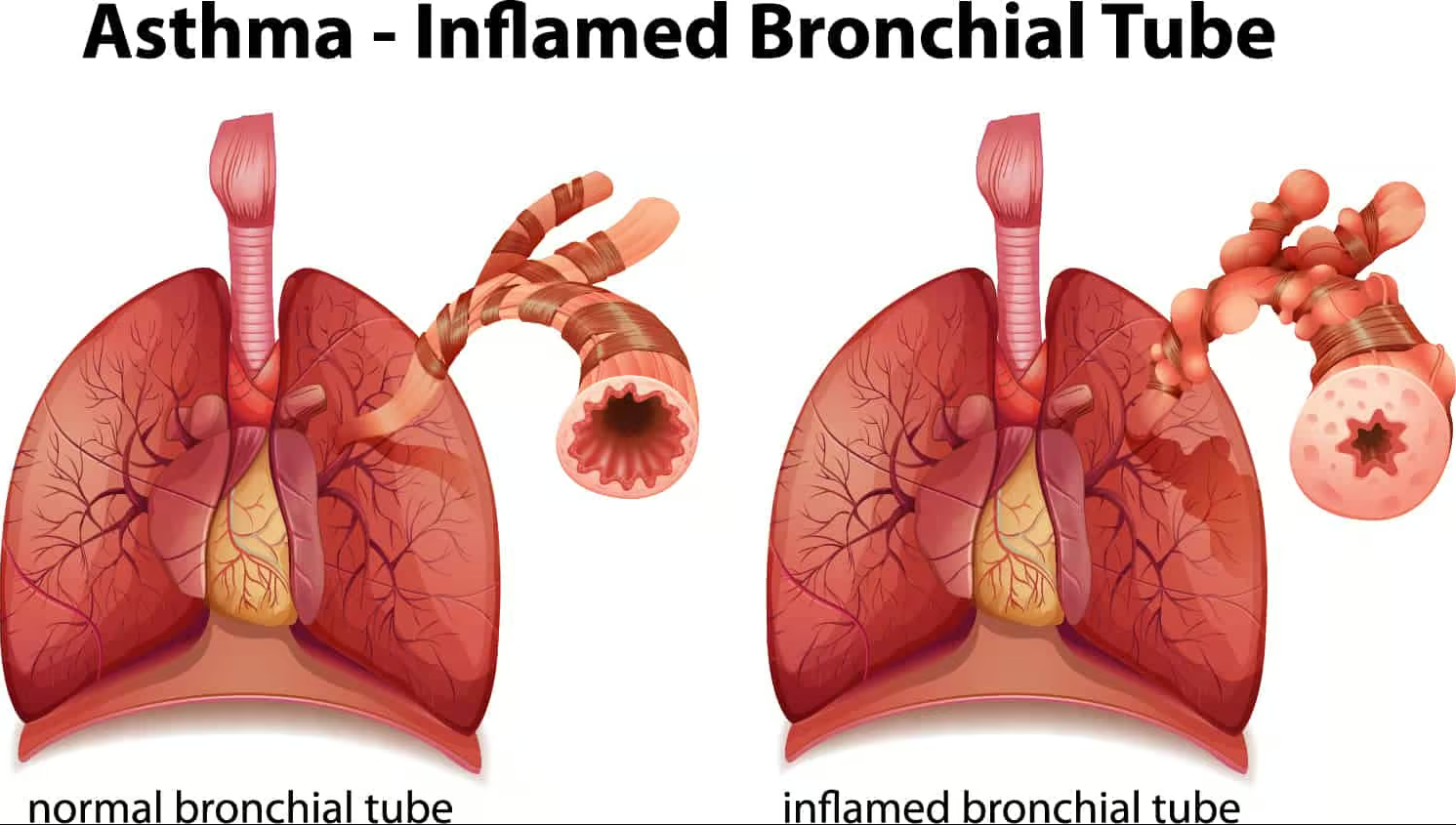 |
Furthermore, it’s observed that children with allergies often follow a path where their allergic conditions progress over time. Notably, those diagnosed with allergic rhinitis (AR) may also develop asthma , as these two conditions are closely linked, collectively referred to as united airway disease. Additionally, allergic conditions tend to co-occur with other immunopathological issues due to compromised immune function.
Allergic individuals also exhibit a weakened type 1 immune response, which is crucial for fighting infections. As a result, children with allergies typically experience infections that are more persistent compared to their non-allergic counterparts.
Given these considerations, it becomes evident that AR and similar allergic conditions necessitate careful attention and management. Medication plays a crucial role in the treatment plan for those with allergies. However, due to the potential for long-term or chronic symptoms, there is a risk of side effects from continuous pharmacological treatment, a concern that is especially pertinent for children. Consequently, there’s a growing inclination towards integrating complementary therapies into the overall treatment strategy. Among these, nutraceuticals are increasingly discussed and utilized by healthcare professionals and parents alike, offering an alternative or adjunctive approach to conventional medication.
| Nutriceuticals |
|---|
 |
The concept of “nutraceutical” emerges from blending “nutrition” and “pharmaceutical,” crafted to denote substances that offer health-enhancing qualities. These substances are usually extracted from foods and can be incorporated into enriched foods or dietary supplements. Nutraceuticals embody the dual advantage of providing nutritional and pharmaceutical benefits, derived from natural food sources with the aim of supporting health beyond mere nutrition. Their rising popularity stems from their potential in the prevention and management of various health conditions. Nutraceuticals are categorized based on their health functions and disease treatment potentials. However, it is crucial to understand that nutraceuticals should not replace conventional medical therapy but may serve as complementary options.
| Dietary supplements |
|---|
 |
Dietary supplements, in this context, are defined as food products designed to enrich the standard diet. They are concentrated sources of nutrients or other compounds that have a nutritional or physiological impact, whether taken individually or combined. These supplements are available in various forms, including capsules, tablets, powders, and liquids, all intended for measured intake. This definition highlights their role in complementing the diet with additional nutrients or beneficial substances in a controlled, dose-specific manner.
Table 1 succinctly presents the most frequently used ingredients in clinical settings for nutraceuticals. It’s essential to remember that nutraceuticals, unlike pharmaceutical drugs, do not provide immediate symptomatic relief and may take a significant amount of time to manifest benefits. They are not intended to replace standard medical treatments but can serve as complementary or preventive measures when used appropriately and within certain guidelines.
Table 1
| Class | Representaive |
|---|---|
| Vitamins | Vitamin C, Vitamin D, Vitamin E, β-caroten |
| Polyphenols | Resveratrol, Catechins (green tea), Curcumin, Rosmarinic acid,Gingerol |
| ω − 3 fatty acids | Fish oil, flaxseed oil |
| probiotics | Lactobacilli, Bifidobacteria strains |
| Prebiotics | Inulin, FOS (fructo-olygosaccharides) |
| Postbiotics | Short chain fatty acids |
| Oligo-elements | Selenium, Zinc, Iron |
| Flavonoids | Quercitin, rutin, spirein |
| Immunomodulants | Lactoferrin, Melatonin, Glucans |
Firstly, it is vital that these products are safe and manufactured by reputable firms. The origin and processing methods of each component must be transparent, especially with probiotics, where only strains with proven benefits and safety profiles should be recommended by healthcare providers. The term “probiotic” itself is broad and demands a precise understanding.
Secondly, the effectiveness of a nutraceutical is closely tied to its dosage. Many products with multiple components offer doses too small to be effective. Healthcare professionals must ensure that the nutraceuticals they recommend contain sufficient amounts of active ingredients to be beneficial.
Lastly, the duration of use is a critical factor to consider. Nutritional supplements often require an extended period to produce noticeable health improvements.
Therefore, when considering nutraceuticals, healthcare providers must conduct a thorough evaluation of the components, their dosages, and the recommended duration of use, akin to the consideration given to any pharmacological treatment.
In conclusion, nutraceuticals hold potential benefits in the management of allergies in children. However, it is crucial for healthcare professionals to prescribe dietary supplements that are backed by documented evidence of their efficacy and safety. By selecting products with proven health benefits, doctors can ensure that these supplements serve as a valuable addition to traditional treatment methods, potentially enhancing the overall management strategy for allergic conditions in children.
References
- Does allergy decrease with age?
- A comprehensive review on natural products caused allergy and its mechanism
- Mechanisms and Practical Use of Biologic Therapies for Allergy and Asthma Indications
- Deciphering the black box of food allergy mechanisms
- Molecular and cellular mechanisms of food allergy and food tolerance
- Mechanisms that define transient versus persistent food allergy
- Seafood allergy: Occurrence, mechanisms and measures
- Recent advances in cellular and molecular mechanisms of IgE-mediated food allergy
- Immunologic mechanisms associated with STAT6 gain-of-function variant identified in early-onset allergies
- An overview of the fundamental immune mechanisms of food allergy
- Mechanisms of Allergy
- Mechanisms of IgE-mediated allergy
Share
Tags
Counters